Tags
[updated 23 May 2026. See tailpiece]
Not for the first time, NSW Premier Chris Minns has again called for the Albanese government to make significant cuts to tobacco excise tax. He’s now been joined by Nick Coatsworth, someone whose previous contributions to tobacco control policy are elusive. Cutting tobacco tax has now become an established factoid: a prescription repeated so often by lazy journalists who’ve not done the calculations, opposition commentators and callers to radio stations that it is obviously the solution to Australia’s rampant illegal tobacco trade.
Anyone can see, right, that if the price of tax-paid cigarettes could be reduced to make them competitive with untaxed illegal cigarettes, smokers would walk away from the untaxed cheapies and drive them out of the market.
Chris Minns and other politicians in this chorus are used to overseeing multi-billion dollar state financing involving eye-watering elaborate forecasting and modelling. But when it comes to tobacco tax, basic primary school arithmetic appears beyond them.
When those calling for excise reduction move to the next obvious question of the size of their sensible tax cut, a common level proposed is the 2020 rate, a so-called “sweet spot” which preceded the explosion in illegal selling that commenced shortly after. So if we dropped it to there, that would fix the problem, right?
Let’s do the maths.
Australia’s tobacco tax since March 3 this year has been $1.52829 per stick, so $30.57 in tax per pack of 20. In March 2020, excise was $0.94964 or $18.99 per pack. If we take a common fully taxed budget brand now costing $42, this would mean the taxed price would drop by $11.58, the difference between $30.57 and $18.99. So our currently $42 retailed pack would cost $30.42 under this tax-slashed proposal.
Deakin University criminologist James Martin has gone a step further, telling the Singapore Straits Times that Australia should consider ditching tobacco tax altogether. This interesting proposal would place Australia with Kuwait and Brunei, where male smoking is 37% and 27% respectively, levels we’ve not seen in Australia for over 40 years.
if the government was to heed Martin’s tax nostrum tomorrow, a typical taxed budget brand costing $42 would then cost $11.43. So would that do the trick and drive illicits out of business?
In Australia, the price today of an illegal, untaxed pack can be as low as $7 if bought by the carton. So a tax drop to 2020 levels would mean a smoker would fork out $30.57, $23.57 or 3.4 times more than they could buy a cheap $7 illegal pack across the road at their nearest illegal tobacconist.
If the government changed Australia’s name to La La Land and axed all tobacco tax, an illegal untaxed $7 pack would still cost $4.43 less per pack than a legal untaxed pack at $11.43.
On either scenario, no budget conscious smoker would ever consider such reductions remotely attractive while illicit cigarettes were still readily available at far less cost.
And let’s remember that a $7 illegal pack includes margins for retailers, transportation from overseas, warehousing and distribution to the retailers, but clearly packs could sell for even less and still remain highly profitable to the criminal syndicates bringing them in.
So how much lower could the illegal price fall? Cambodia is a well-known transit hub for illegal tobacco smuggling. A pack of cigarettes, including local taxes, can be bought there for just 34c. Add margins for illegal retailers, transportation from overseas, warehousing and distribution to the retailers, and there will still be plenty of fat that will allow packs prices to fall far lower than $7.
Globally, there are many examples of nations with very low tobacco tax and very high levels of illicit trade. So if high tobacco tax explains high illicit trade, how is it that so many low taxing countries are awash with black market cigarettes too? Simplistic causal attributions about high tobacco tax clearly hold low generalisable explanatory power about what is a global problem which has often seen the major involvement of established tobacco transnationals.
For decades there have been huge global gaps between official tobacco export and import data. The gaps are explained by large volumes of exports arriving in transit countries where corruption facilitates re-export via illicit trade without any tax being levied.
Australia’s Border Force has intercepted nearly a kilotonne of illegal tobacco and 4 million vapes since December 2025. Three state governments have closed 260 illegal tobacco shops for a total of 13,000 days in Queensland, NSW has closed 250 for 22,500 days since November 2025, including 10 in Sydney’s Haymarket just last week and South Australia got out of the blocks first with 100 closures between June and November 2025.
These penalties, which can also include massive fines and gaol times, are radically changing the risks and costs of engaging in illicit trade in Australia. No country has zero illicit tobacco trade, but those calling for reduced tax are in knowing or gormless lockstep with Big Tobacco which has routinely lobbied government to lower the tax for years to increase their own margins.
Tailpiece: John Menadue’s blog, Pearls and Irritations, republished this blog here on May 19. It caught the eye of the lugubrious vape promoter Dr Alex Wodak who reached into his deep lexicon of nastiness (see an earlier blog here), declaring on his BlueSky feed this garbled rubbish (“rather than argument and big smear” …what???) :
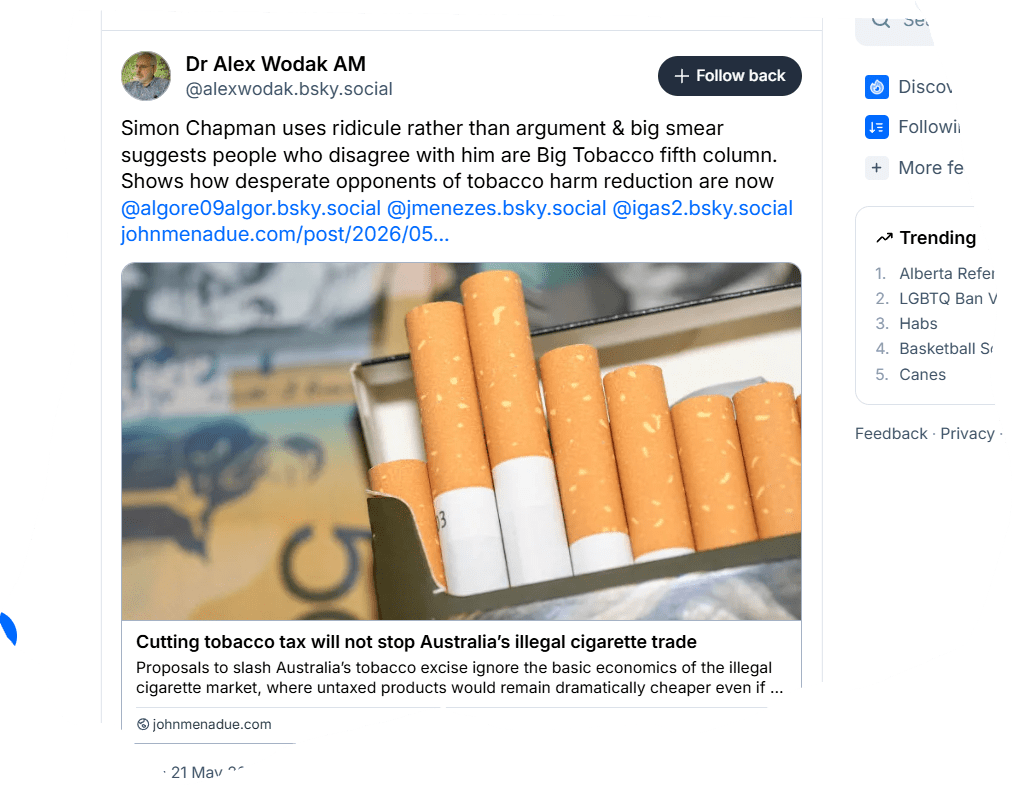
Fresh from a 2025 invited tour of British American Tobacco’s “innovation centre” in Southampton, Wodak recently made a doorstopper submission to the recent Australian Senate Enquiry into illicit tobacco.
Across 21 pages, he helpfully included no less than 17 screenshots from Philip Morris and Altria reports to make his argument that reduced harm products like vapes would lead nations away from smoking, a position identical to that of Big Tobacco companies. You could almost feel the love. Invited study tours of Philip Morris innovation centres can surely not be far off.
Odd then indeed that many nations awash with vaping thanks to liberal access policies have not seen them sweep past Australia’s smoking prevalence rate, as I argued with colleagues here.
Odd then too, that with all the years of all this innovation, British American Tobacco still rakes in 82% of its revenue from combustible tobacco. And no tobacco company – unlike car manfacturers transitioning from fossil fuel powered cars to electric vehicles – has yet to name a date whe they will stop making cigarettes.