Tags

Photo credit: Lindsay Fox
Vaping advocates eat, live, breathe and rejoice in their nicotine addiction. But in 2024, they lost the political debate on vaping policy when the Australian Senate voted to make vapes only legally accessible through pharmacies.
You could hear their wailing deep into the night. This heinous decision would make accessing vapes hugely difficult, they swore. It was gently pointed out that Australians make 440m annual visits to some 5000 pharmacies, an average of 18 times per year, walking out with 331m subsidised prescriptions. So onerous that vapers should have to go to such lengths.
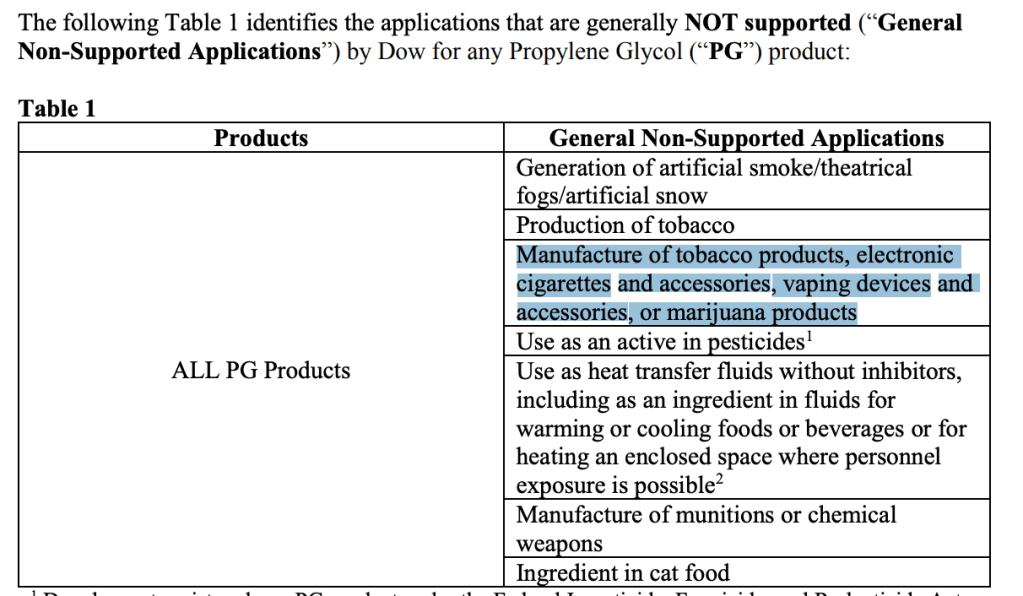
They then retorted that the tiny range of allowed flavours were massively unappealing. They’d lost the parliamentary vote, but will never stop insisting that, unlike every inhalable drug in the global pharmacopeia where flavours have never been allowed for safety reasons, it’s just fine with vapes. It’s not OK to inhale flavouring chemicals in lifesaving therapeutics, but it’s quite OK to do that hundreds of times a day when you vape. Makes perfect sense eh?
The two main vaping advocacy groups, the Australian Tobacco Harm Reduction Association (ATHRA) and Legalise Vaping Australia both put up their white flags quietly and shut down. Those remaining are tiny inconsequential echo chambers.
But the recent focus on Australia’s massive illegal tobacco and vape trade has acted like smelling salts to a few punch drunk vaping advocates who were down on the canvas. They are now disporting themselves in new white hero hats holding aloft their messianic vision that the time is now right for the government to repeal its galactic folly on pharmacy-only vape access.
If vapes could be re-liberated from pharmacies and made available through all those highly responsible tobacconists, vape shops and convenience stores (who have never been known to break the law by selling illicit tobacco or selling to kids), many smokers who for the last 12 years have apparently never heard of vapes let alone tried them, would have the tape peeled from their eyes. En masse, they would discard their cheap cigarettes and storm into vape stockists. Smoking prevalence would drop like a stone.
There are a couple of teensy-weensy problems with these wide-eyed fantasies.
First, almost every illegal tobacco shop across the country – and there are thousands — is also stocking illegal vapes and have been doing so for at least four years. The vaping advocates’ dream is already a reality with a huge number of stockists and the cornucopia of flavours they lie awake dreaming of. This being the case, why then haven’t we already seen an avalanche of smokers switching to vapes? Shouldn’t we be seeing vaping going through the roof already?
Not quite.
Second, there are many countries where the very policies that these fantasists dream of are a reality, for many years. Vapes are freely available in much of Europe, across the USA, in Canada, the UK and New Zealand. And sorry to mention this, illegal tobacco also proliferates.
This being the case, it should be obvious that smoking prevalence in such nations should be embarrassing the socks off Australia, right?
Let’s then take a look at data in a range of countries around the time that Australia’s most recent national data on smoking and vaping was published (the next data will be ready by the end of 2026)

It’s clear that New Zealand is an outlier here: the other comparator regions have similar smoking prevalence, with the Smoking Toolkit Study estimate for England being higher and that for Europe much higher. Similarly striking is Hong Kong: despite banning the sale and public personal possession of vapes, it has just reported a 2025 smoking prevalence of 8.5%, down from 9.1% in 2023.
With highly liberal vape retail access across the past decade occurring as much, if not more, in England, USA and Canada as in New Zealand, and smoking prevalence in all these nations declining, any putative causal generalisation about the downward effect on smoking of liberal versus restricted vape access as in Australia becomes immediately contentious. If liberal access to vaping sees smoking fall across populations, why are not all liberal access nations’ smoking rates much lower than Australia’s after at least a decade of widespread use and liberal access?
And then there’s this bell ringer. In nations where data are available, there are 45 nations which have smoking prevalence under 10%. Just one of these nations (New Zealand) has liberal vape access policy. The rest don’t. So much for the vaping theology that vaping is somehow necessary to reducing smoking to rock bottom.
Other blogs in this series
Vaping theology: 1 The Cancer Council Australia takes huge donations from
cigarette retailers. WordPress 30 Jul, 2020
Vaping theology: 2 Tobacco control advocates help Big Tobacco. WordPress 12 Aug, 2020
Vaping theology: 3 Australia’s prescribed vaping model “privileges” Big Tobacco WordPress Feb 15, 2020
Vaping theology: 4 Many in tobacco control do not support open access to vapes because they are just protecting their jobs. WordPress 27 Feb 2021
Vaping theology: 5 I take money from China and Bloomberg to conduct bogus studies. WordPress 6 Mar, 2021
Vaping theology: 6 There’s nicotine in potatoes and tomatoes so should we restrict or ban them too? WordPress 9 Mar, 2021
Vaping theology: 7 Vaping prohibitionists have been punished, hurt, suffered and damaged by Big Tobacco WordPress 2 Jun, 2021
Vaping theology: 8 I hide behind troll account. WordPress 29 Jun, 2021
Vaping theology: 9 “Won’t somebody please think of the children”. WordPress 6 Sep, 2021
Vaping theology: 10: Almost all young people who vape regularly are already smokers before they tried vaping. WordPress 10 Sep, 2021
Vaping theology: 11 The sky is about to fall in as nicotine vaping starts to require a prescription in Australia. WordPress 28 Sep, 2021
Vaping theology: 12 Nicotine is not very addictive WordPress 3 Jan 2022
Vaping theology 13: Kids who try vaping and then start smoking,would have started smoking regardless. WordPress 20 Jan, 2023
Vaping theology 14: Policies that strictly regulate vaping will drive huge
numbers of vapers back to smoking, causing many deaths. WordPress 13 Feb, 2023
Vaping theology 15: The government’s prescription vape access scheme has failed, so let’s regulate and reward illegal sellers for what they’ve been doing. WordPress 27 Mar 2023
Vaping theology 16: “Humans are not rats, so everybody calm down about nicotine being harmful to teenage brains”. WordPress 13 Jul, 2023
Vaping theology 17: “Vaping advocates need to be civil, polite and respectful” … oh wait. WordPress 3 Oct, 2023
Vaping theology 18: Vaping is a fatally disruptive “Kodak moment” for smoking. WordPress Oct 30, 2023
Vaping theology 19: Vaping explosions are rare and those who mention them are hypocrites. WordPress 17 Nov, 2023
Vaping theology 20 : Today’s smokers are hard core nicotine dependent who’ve tried everything and failed – so they need vapes. WordPress 14 Dec, 2023
Vaping theology 21: Australia’s prescription vapes policy failed and saw rises in underage vaping and smoking. WordPress 10 Jan, 2024
Vaping theology 22: “Prohibition has never worked at any point for any other illicit substance”. WordPress 17 Mar 2024
Vaping theology 23: “84% of the Australian public are opposed to the way the government will regulate vapes” WordPress 2 Apr, 2024
Vaping Theology 24: “Tobacco control advocates are responsible for vape retail store fire bombings and murders. WordPress 27 May, 2024
Vaping theology 25: Vaping is as harmless as breathing in stream. So everyone relax. 10 tenets of vaping harm denial.WordPress 10 Mar, 2026